About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。


 Dual Primary Lung and Breast Cancer: Choosing the Right Approach to Regain Hope for Survival .
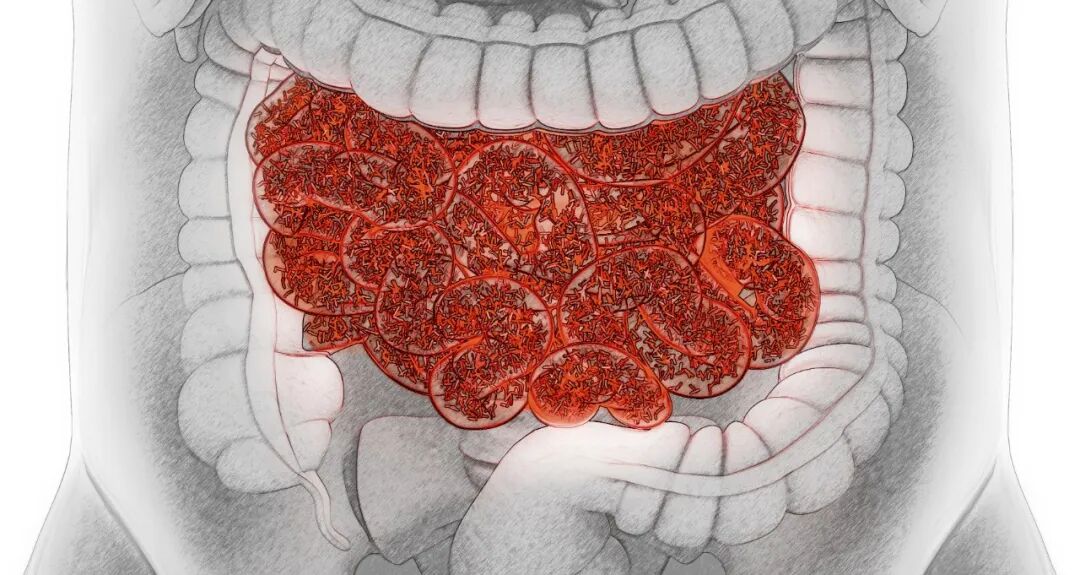
Dual Primary Lung and Breast Cancer: Choosing the Right Approach to Regain Hope for Survival . Colorectal cancer (CRC) has an annual incidence rate of 1.3 million new cases globally, making it the third most common malignant tumor worldwide. In most regions, the incidence rate in males is significantly higher than that in females, and it is also the second leading cause of cancer-related deaths globally. The incidence rate of CRC in China currently ranks third. In 2011, the incidence rate of CRC in China was 23.03 per 100,000 people. Many studies have confirmed that the incidence of CRC is shifting towards younger age groups, with the number of cases among young people gradually increasing over the past decade.
Among the various mechanisms underlying the development of CRC, colorectal adenoma (CRA) is a significant factor. According to the adenoma-carcinoma sequence hypothesis, which describes the development pattern of normal mucosa-adenoma-carcinoma, 85% of intestinal cancers develop from adenomatous polyps.
CRA can progress from low-grade dysplasia to tumor cells. Depending on different histopathological classifications, polyps can be divided into adenomatous and non-adenomatous types. Adenomatous polyps can further be classified into tubular adenomas with less than 20% villous component, tubular-villous adenomas (also known as mixed adenomas) with 20% to 80% villous component, villous adenomas with more than 80% villous component, and less common serrated adenomas.
In advanced adenomas, a higher villous component is a high-risk factor for the development of CRC. Tubular-villous adenomas have the potential to develop into invasive cancers. Therefore, early screening, diagnosis, and intervention of precancerous lesions are particularly important. Endoscopic resection of adenomas can effectively prevent CRA from progressing to CRC and improve public health.
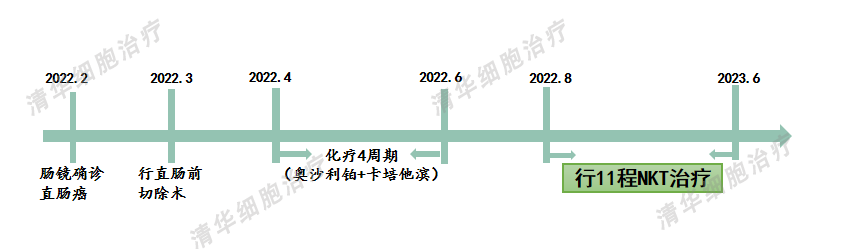
After reviewing Ms. Shan's medical records, Professor Zhang Minghui made the following analysis and judgment:
2. The patient, being elderly, has undergone surgery and chemotherapy, which have caused significant damage to their immune system. Restoring immunity as soon as possible is of utmost importance.
3. The patient has dual primary cancers of breast cancer and rectal cancer, and a cancerous constitution requires heightened vigilance.
4. vNKT therapy utilizes powerful immune cells to eliminate tumor cells that may remain undetected in the body, with essentially no side effects, and can reduce the risk of tumor recurrence.

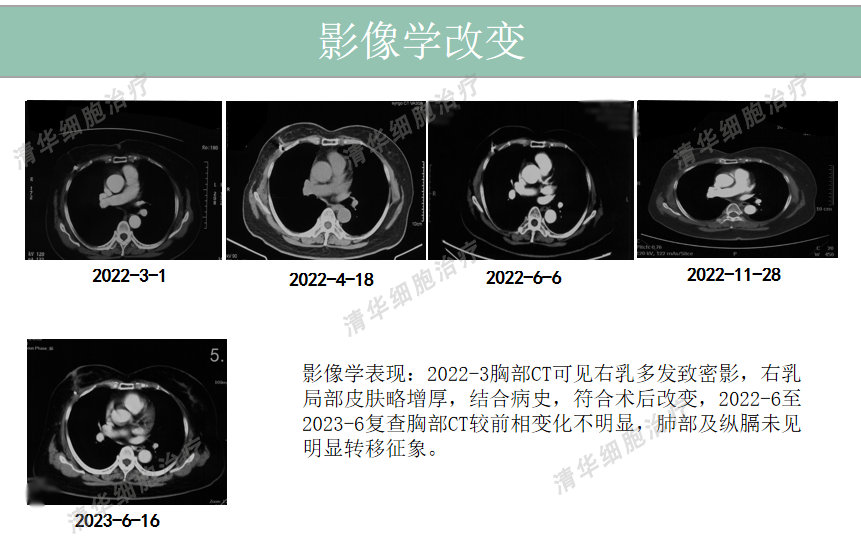


References:
Click on the image