About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。
 Ms. G is suffering from a relatively rare type of soft tissue sarcoma (Ewing's sarcoma). Sarcomais different from cancer, but both belong to malignant tumors. The primary difference between sarcoma and cancer lies in the origin of the tissue. Cancer is a malignant tumor that originates from epithelial tissue, while sarcoma is a malignant tumor that originates from connective tissue, muscle, and other tissues, hence the term "sarcoma".
Ms. G is suffering from a relatively rare type of soft tissue sarcoma (Ewing's sarcoma). Sarcomais different from cancer, but both belong to malignant tumors. The primary difference between sarcoma and cancer lies in the origin of the tissue. Cancer is a malignant tumor that originates from epithelial tissue, while sarcoma is a malignant tumor that originates from connective tissue, muscle, and other tissues, hence the term "sarcoma". 
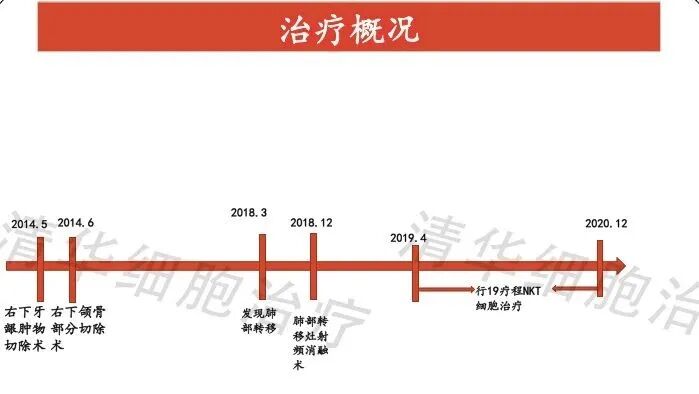
The patient discovered a painless mass in the right lower gum in March 2014, measuring approximately 2*1cm. On May 17th, an outpatient surgical excision was performed. Pathology indicated a spindle cell tumor in the right lower posterior region of the tooth, involving bone tissue. One lymph node was removed and no metastasis was found, suggesting a need for external consultation.

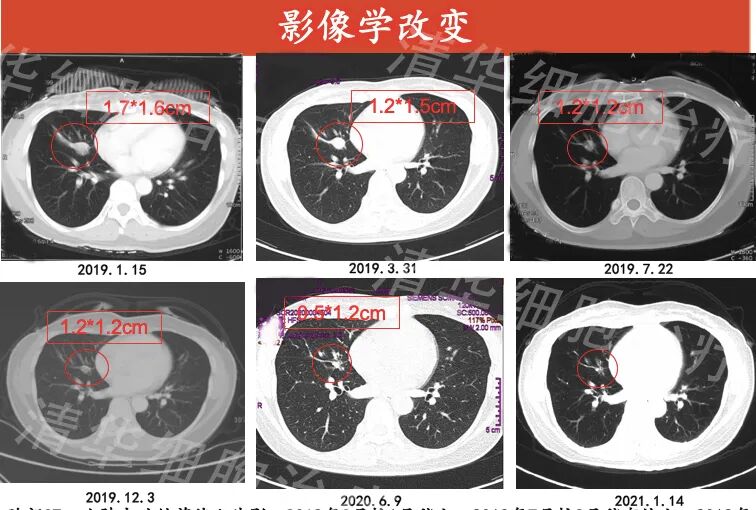
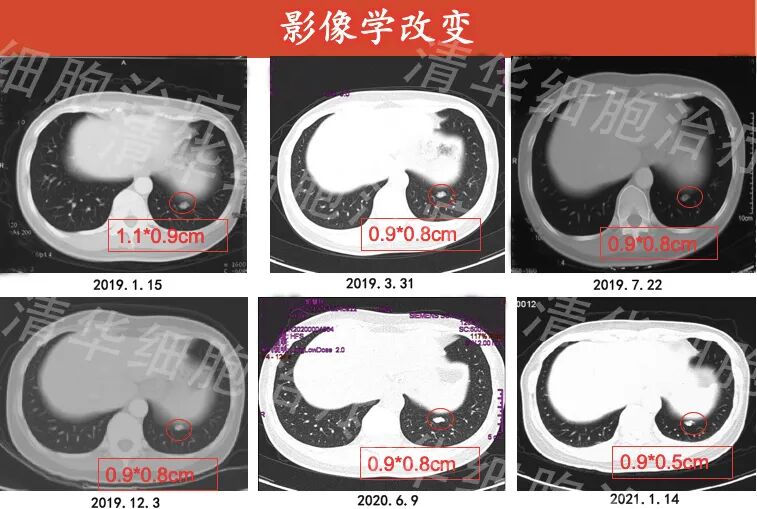
Chest CT: nodules in the left lower lobe of the lung with uneven density, calcification visible within, slightly reduced in size from March 2019 compared to January 2019, no significant change from March 2019 to June 2020, and slightly smaller in January 2021 compared to June 2020.
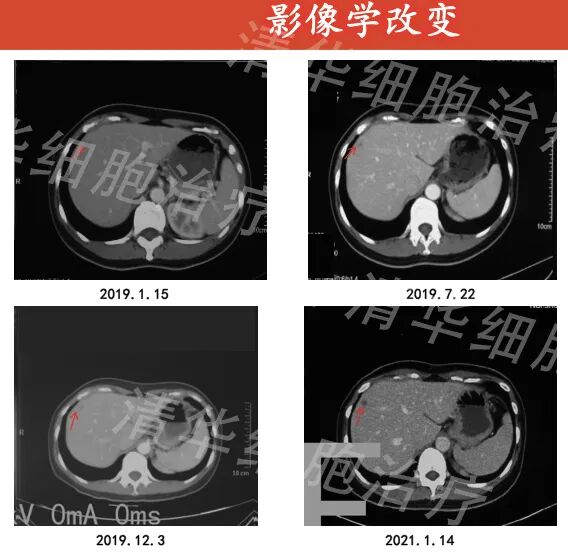
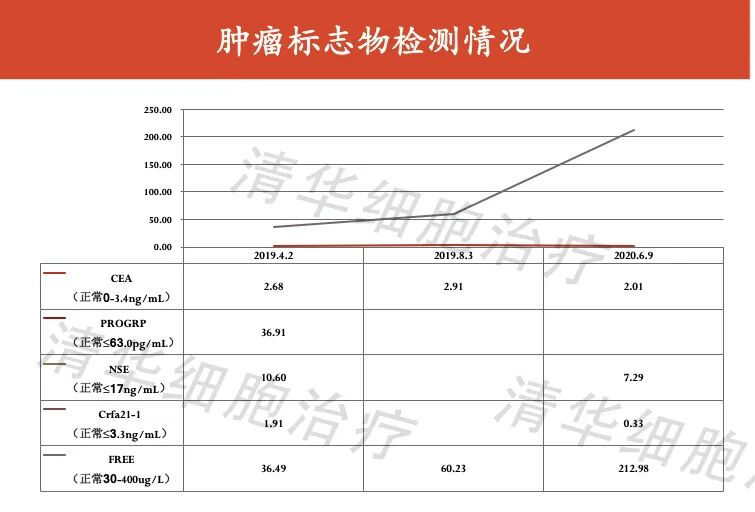
From April 2019 to August 2021, all tumor markers tested were within the normal range and remained stable. After NKT treatment, with the reduction of tumor burden, the patient's quality of life improved significantly, with a weight gain of 1-3kg, good sleep and appetite, and a quality of life score of 92 points.
Ms. G underwent 21 courses of NKT cell immunotherapy, with almost no visible maximum metastatic lesion in the lungs, and the remaining smaller metastatic lesions either shrank or remained unchanged. No new signs of disease progression were observed in other organs. Her progression-free survival (PFS) reached 27 months, and she continues to receive treatment and follow-up.
NKT Classic Case Review
Click on the image
