About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。

For the same gastric cancer, why do some people manage to survive for 6 years and achieve a cure, while others only live a few months from diagnosis to death? Apart from the inherent difficulties in controlling the disease itself, the formulation of treatment strategies is also crucial in determining the success of treatment. Should chemotherapy come first or surgery? Is everything fine after surgery? What other treatment methods can we use? How to prevent recurrence and metastasis? These are all things we need to understand.
What are the reasons behind Mr. Wu's successful treatment and smooth survival for 6 years since his diagnosis of gastric cancer? Let's analyze together and see if there are any lessons worth learning.
Disease Overview
In July 2018, Mr. Wu initially experienced symptoms of dysphagia to some extent, and he was worried about the possibility of esophageal issues. A gastroscopy was performed, and the biopsy results showed moderate-to-poorly differentiated adenocarcinoma from the cardia to the lower esophagus. After being diagnosed, Mr. Wu did not immediately undergo surgical treatment. He wished to consult with several doctors and listen to different opinions before making a decision.
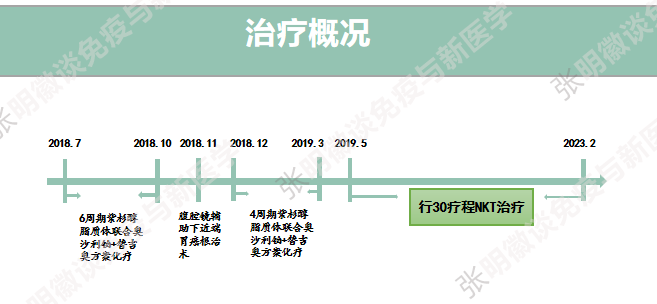
After consultation, Mr. Wu adopted a neoadjuvant chemotherapy regimen consisting of six cycles of paclitaxel liposomal formulation combined with oxaliplatin and temozolomide, i.e., systemic chemotherapy was initiated before the implementation of local treatment (surgery). After completing the neoadjuvant chemotherapy in November 2018, Mr. Wu underwent laparoscopic proximal gastrectomy under general anesthesia, followed by four cycles of adjuvant chemotherapy with the same regimen.
Postoperative pathology indicated tumor infiltration into the muscular layer with vascular thrombi, and lymph node metastasis was visible (3/21), whereas vascular thrombi are a high-risk factor. Typically, tumors grow by infiltrating deeply into the gastric wall, and vascular thrombi indicate that cancer cells have infiltrated deep blood vessels. Tumor cells precisely use this method to leave the primary lesion and metastasize to other sites, thus posing a higher risk of recurrence in the future.
What about postoperative risks? [Recommendations for tumor postoperative rehabilitation] can help address them
Facing the risk of recurrence, Mr. Wu didn't dare to take it lightly. While undergoing postoperative chemotherapy, he reached out to Professor Zhang Minghui for tumor postoperative rehabilitation recommendations, hoping to develop a systematic rehabilitation plan tailored to his condition. This plan aimed to gradually recover from the physical trauma caused by surgery and chemotherapy while preventing tumor recurrence and metastasis.
The Lehexin Medical team provided rehabilitation recommendations based on assessment and analysis:
1. The patient adopted a "sandwich biscuit" type adjuvant chemotherapy regimen, which created conditions for conventional radical surgery. The patient's tumor burden was relatively low at this time, providing favorable conditions for vNKT cell therapy.
2. Although the visible tumors were removed, the pathological results still indicated a high risk of recurrence and metastasis due to vascular cancer thrombus and differentiation type. Conventional treatment generally ends at this point, but it cannot guarantee the absence of recurrence and metastasis. To consolidate the early "battle achievements," another effective treatment method was sought - vNKT immune cell therapy.
3. At the same time, positive psychology was incorporated to rebuild psychological state and establish confidence in recovery; dietary adjustments were made to change previous unhealthy lifestyle habits; and physical fitness was gradually restored through qigong practice.
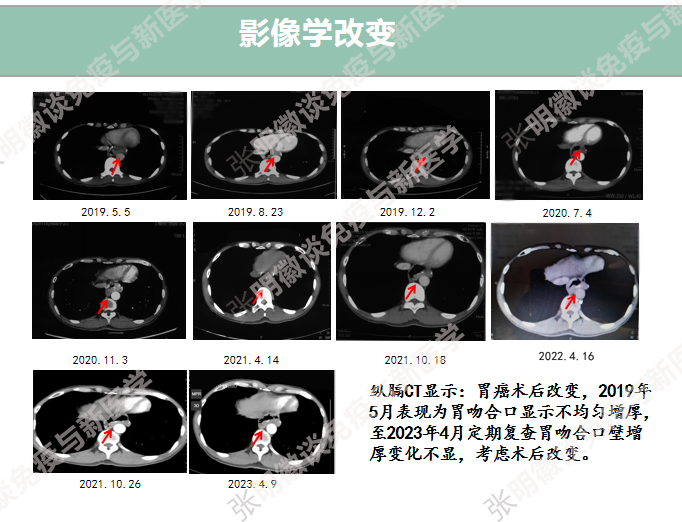
In May 2019, Mr. Wu underwent vNKT cell immunotherapy. The initial regimen was one course per month, and after multiple follow-up examinations, no signs of recurrence or metastasis were observed, leading to a reduction in treatment frequency to one course every two months. As of February 2023, 30 courses have been completed. Mr. Wu has smoothly spent six years and achieved clinical cure.
Analysis and Commentary
Gastric cancer is a common malignant tumor in clinical practice. According to surveys, its incidence rate ranks fifth nationwide, and among all causes of cancer death, it ranks third[1]. The treatment of advanced gastric cancer with radical gastrectomy combined with neoadjuvant chemotherapy has shown good results, reducing the degree of patient body damage, the incidence of complications, and shortening the recovery time. The application of neoadjuvant chemotherapy before radical gastrectomy can inhibit tumor cell activity, control the probability of tumor cell metastasis and diffusion during surgery, and reduce the rate of disease metastasis and recurrence[2]. After comprehensive consideration, Mr. Wu adopted neoadjuvant chemotherapy, which earned him a greater chance of survival. Post-surgery recovery is a key point. Mr. Wu adopted Lehexin Medical's [post-tumor surgery recovery recommendations] to reduce the risk of recurrence, enhance immunity, resume normal work and life, and return to society.
Therefore, I hope that patients do not seek treatment in haste and leave regrets in their treatment. If you are unable to make a decision on the path of disease treatment, you can listen to Lehexin Medical's [post-tumor surgery recovery recommendations] and contact the assistant for advice.

Contact Us
Scan QR Code
Communicate with Professor Zhang Minghui's Team
Reference Source:
[1] Wang Shaoming, Zheng Rongshou, Han Bingfeng, et al. Analysis of the Age Characteristics of Incidence and Mortality of Malignant Tumors in the Chinese Population in 2022 [J]. China Cancer, 2024, 33(03):165-174.
[2] Liu Zhuang Clinical Effect Analysis of Radical Gastrectomy Combined with Neoadjuvant Chemotherapy for Advanced Gastric Cancer [J]. China Modern Drug Application, 2023, 17(22):112-114. DOI: 10.14164/j.cnki.cn11-5581/r.2023.22.030.
Edited/Typeset by: Zhao Runquan
Medically Reviewed by: Wang Ying