About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。

If you cannot understand the subsequent professional description, you can finish reading this text in two minutes
Disease Overview
knowledge
Immunohistochemistry of breast cancer
Her-2, whose full name is human epidermal growth factor receptor 2, is a proto-oncogene. When the HER-2 gene is highly expressed in cancer cells, excessive HER-2 protein will be produced on the cell membrane, stimulating the rapid growth of cancer cells and increasing their invasiveness. Therefore, patients with HER-2 positive breast cancer have a more dangerous condition, are more prone to recurrence and metastasis, and have a shorter survival period, which is clinically referred to as poor prognosis. However, targeted therapy for HER-2+ can improve the patient's chances of survival.
ER and PR stand for estrogen receptor and progesterone receptor, respectively. Patients who are positive for both ER and PR can undergo endocrine therapy in addition to chemotherapy after surgery, which can greatly extend their survival period and improve their prognosis.
If ER, PR, and Her-2 are all negative, it is what we commonly refer to as triple-negative breast cancer, for which treatment options are limited. It is insensitive to both targeted therapy and endocrine therapy, and the prognosis is poor.
1. Although the patient underwent radical surgery and the primary visible lesion was removed during the operation, the presence of intravascular cancer thrombus indicates a high risk of postoperative metastasis.
2. The patient's ER and PR status are negative, making endocrine therapy inapplicable. Postoperative chemotherapy and targeted therapy have been completed, and conventional treatment typically ends here.
3. To achieve long-term stability, NKT therapy can be adopted to eliminate potentially invisible tumor cells. Additionally, NKT therapy has almost no side effects, significantly reducing the risk of metastatic recurrence.
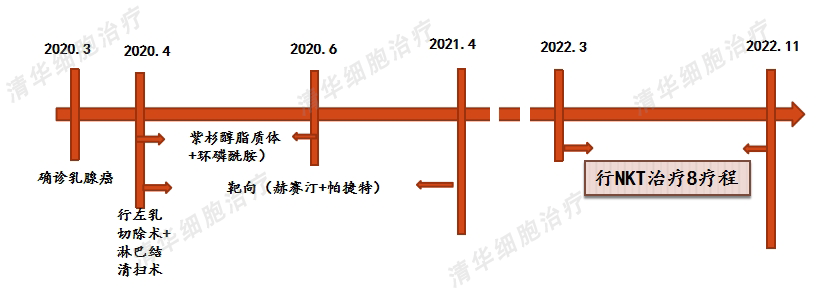
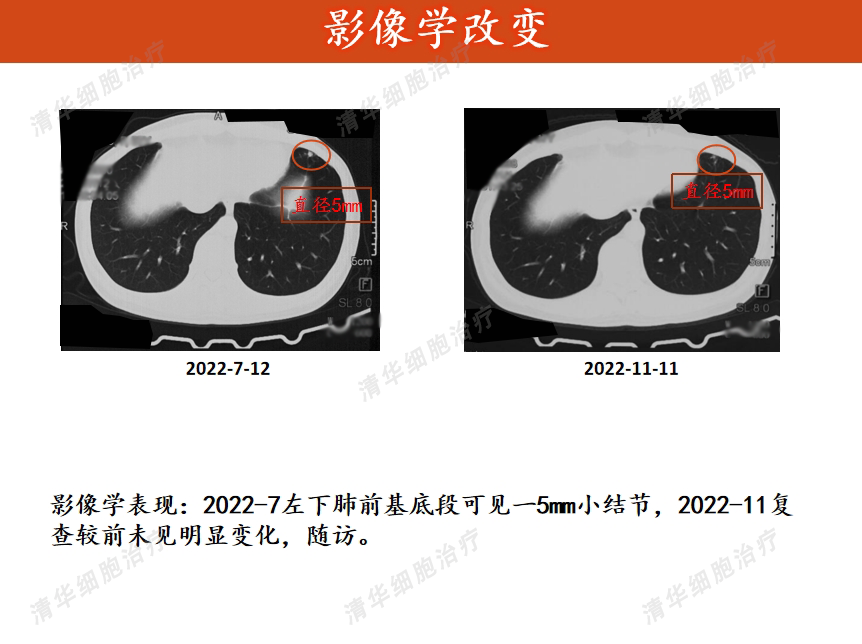
From March 2022 to November 2022, Ms. Li completed the first phase (8 courses) of treatment. During this follow-up examination, no clear signs of tumor recurrence were observed, and her overall condition remains stable.
Imaging
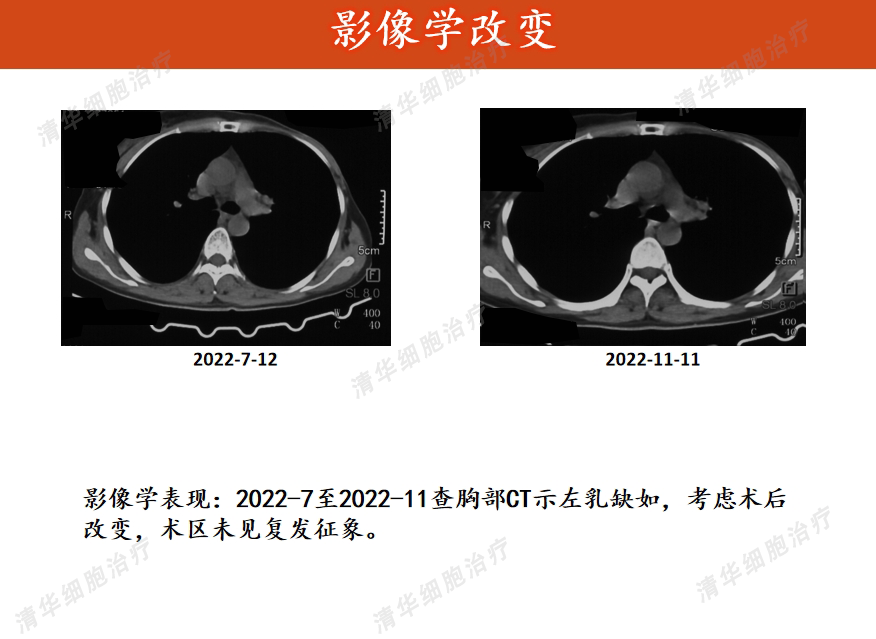
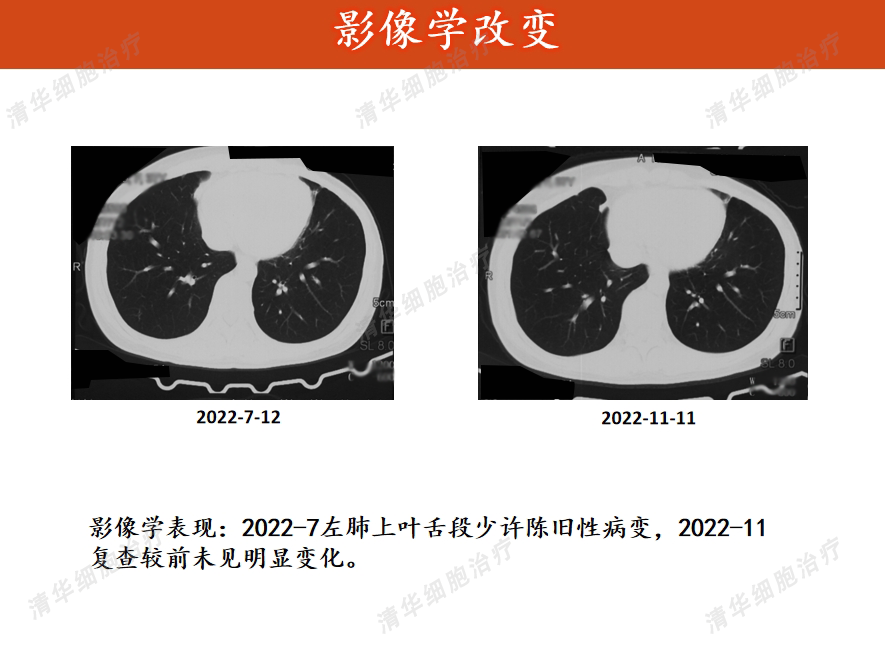
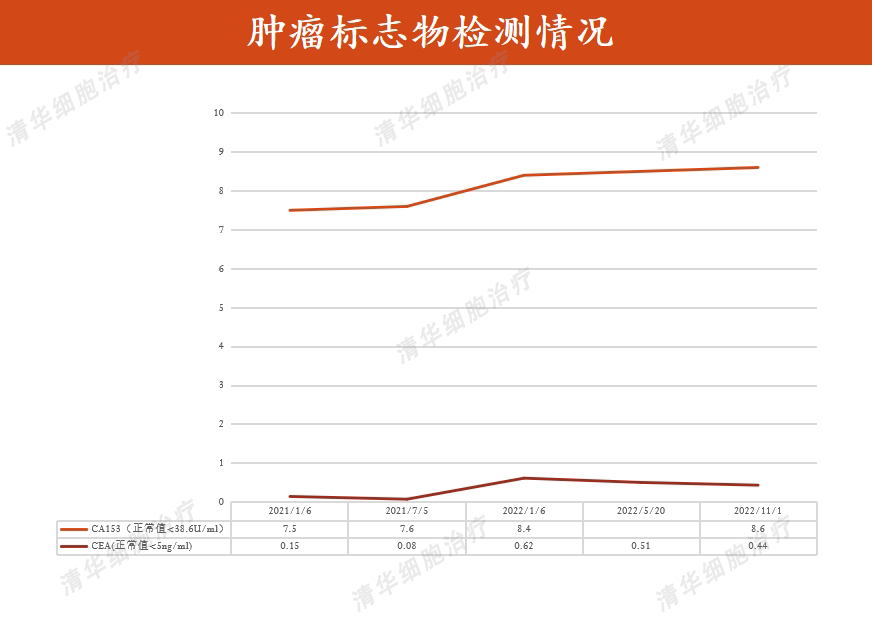
Tumor markers
Conclusion and Comments
Reference:< H335>
Click on the image