About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。


This method involves inserting a tube from the femoral artery in the lower limbs or the radial artery in the upper limbs to reach the liver, blocking the artery supplying the tumor, and causing ischemic necrosis of the tumor.
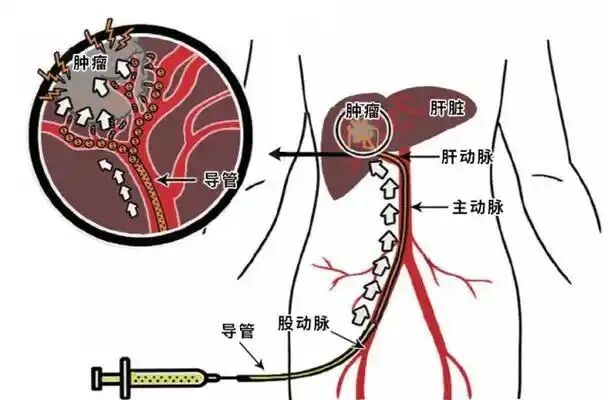
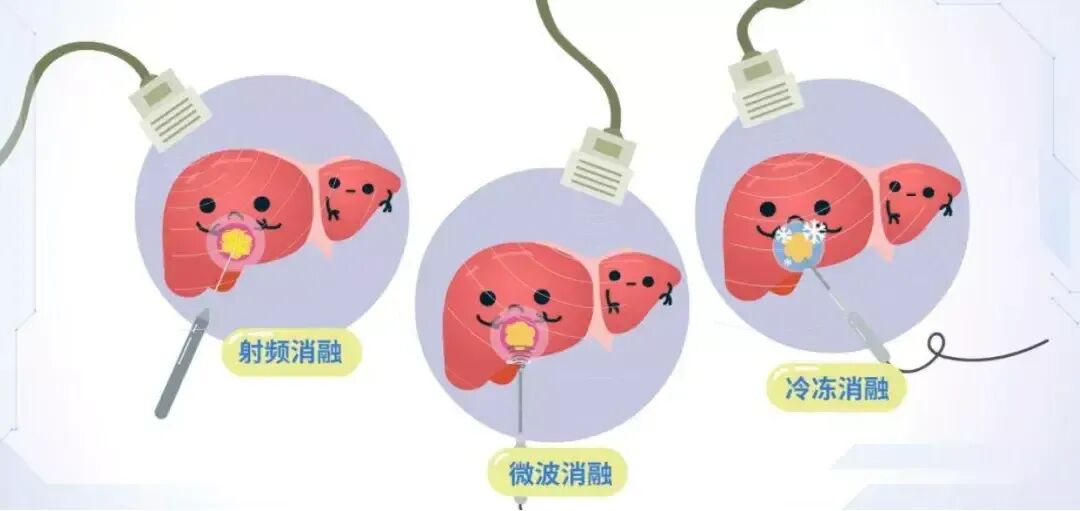
Overview of the illness
Mr. Feng, the patient, was found to have two lesions in his liver during a physical examination in March 2019: a 1.7*1.9cm lesion in the left liver and a 0.4*0.5cm lesion in the right liver, with a suspected malignant tumor in the left liver. On April 24, 2019, he underwent left lateral segmentectomy of the liver and cholecystectomy. Postoperative pathology revealed: (liver) hepatocellular carcinoma, moderately differentiated, Edmondson grade: III; tumor size 2X1.7X1.1cm, without involvement of the liver capsule; no cancer at the resection margin; surrounding liver tissue consistent with chronic viral hepatitis B G1, S3. Immunohistochemistry: cancer tissue: GPC-3(3+), Hepatocyte (3+), CD34 (diffusely distributed in microvessels), CK19 (-), Ki-67(+40%), p53 (2+), CK7 (1+). Liver tissue: HBsAg(2+), HBcAg (-). From April 2019 to 2020, he was treated with long-acting interferon and Zadaxin.
In 2020, a follow-up examination revealed an enlargement of the right liver lesion (specific details unknown). In November 2020, interventional ablation therapy was performed. On July 15, 2022, an upper abdominal MRI showed changes after resection of the liver lesion and interventional ablation, with a possible recurrence (an abnormal enhanced nodule measuring approximately 14mm*13mm was observed within the ablation lesion in the right lobe of the liver).
On July 22, 2022, a hepatic arteriography and embolization procedure were performed. On July 26, interventional ablation therapy was administered. On September 28, 2022, a PET-CT scan revealed postoperative changes in the left lobe of the liver after partial resection; a low-density lesion with high density in the right lobe of the liver, without metabolic activity, consistent with post-treatment changes in liver cancer, and clinical follow-up is recommended. A high-metabolic lymph node (SUVmax 9.44) measuring approximately 2.0cm x 1.2cm was found adjacent to the right external iliac artery, with a high likelihood of metastasis. On October 4, a pelvic CT scan showed: 1) an enlarged lymph node adjacent to the right external iliac artery, measuring approximately 1.9cm x 1.1cm, considered metastatic based on the patient's history; 2) prostatic calcification. On October 19, 2022, a lymph node resection was performed, and postoperative pathology revealed: frozen section examination (abdominal lymph nodes and surrounding tissues) showed two lymph nodes with reactive hyperplasia. Additional examination (perifascial fat around the inguinal lymph nodes) found four lymph nodes with reactive hyperplasia.
On May 26, 2023, the upper abdominal MR imaging revealed: 1. Postoperative changes following liver lesion resection and interventional ablation, with no clear signs of new or recurrent lesions; 2. Focal perfusion abnormalities in the liver, possibly indicating arteriovenous shunt, and a follow-up examination is recommended.
After reviewing Mr. Feng's medical records, Professor Zhang Minghui made the following second diagnosis and treatment suggestion for Lehe New Medicine:
1. Although the tumor was relatively small at the time of the patient's initial treatment, the lack of effective adjuvant therapy after surgery was the main reason for recurrence. Subsequently, the patient experienced two recurrences, both of which were treated with interventional combined radiofrequency ablation. This treatment method cannot completely eradicate the tumor, making recurrence inevitable. To consolidate the early treatment effects and control recurrence, more effective follow-up treatment measures are needed.
2. Current adjuvant therapy after surgery typically involves drug treatment, such as targeted therapy, chemotherapy (transcatheter arterial chemoembolization, TACE), and immunomodulatory therapy. These treatments can effectively kill and inhibit tumor cells in the short term, but drug resistance cannot be avoided, and long-term efficacy cannot be achieved. Additionally, they have significant side effects, which can damage the immune system, hematopoietic system, and organ function. Therefore, they are not ideal adjuvant therapy after surgery.
3. vNKT therapy can utilize powerful immune cells to eliminate residual or newly emerging tumor cells and reconstruct the immune microenvironment, with essentially no side effects. After completing surgical treatment, the tumor burden is reduced, making it the optimal intervention opportunity. vNKT therapy can effectively reduce the risk of recurrent and newly emerging tumors, making it highly suitable as the main treatment method for Mr. Feng's follow-up treatment.
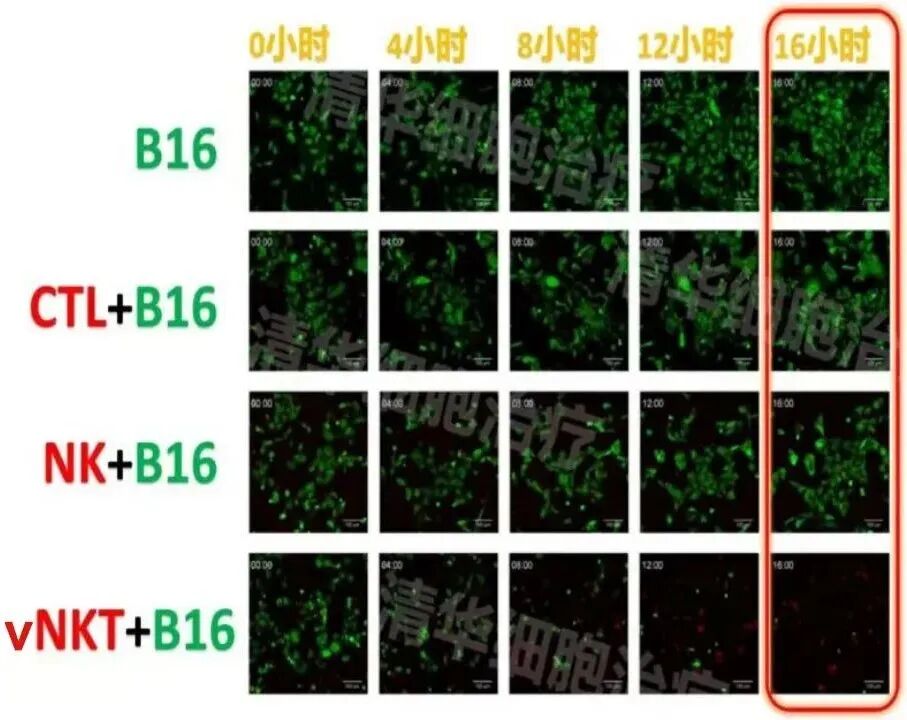
Experimental conditions: In the presence of vNKT cells, after 16 hours, nearly all B16 tumor cells were killed!
Professor Zhang introduced vNKT treatment technology and the treatment outcomes of previous cases in detail to Mr. Feng and his family, and provided detailed answers to Mr. Feng's questions. After thorough communication, he finally obtained the unanimous approval of Mr. Feng and his family. On August 1, 2023, vNKT cell therapy was started, with a regimen of one course per month. By November 1, 2024, 16 courses had been completed. Currently, the patient's condition is stable with no signs of recurrence or metastasis. The patient is in good spirits, with good appetite and sleep, and a good quality of life.
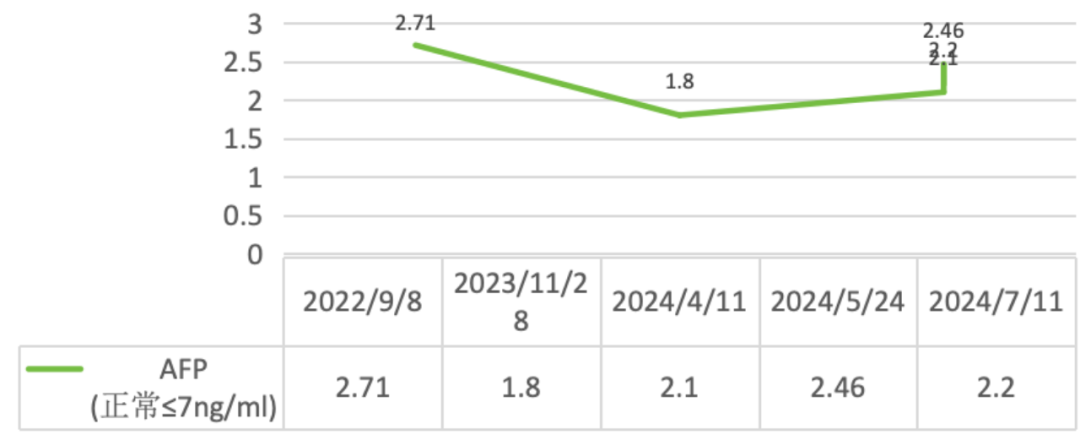
Changes in tumor markers
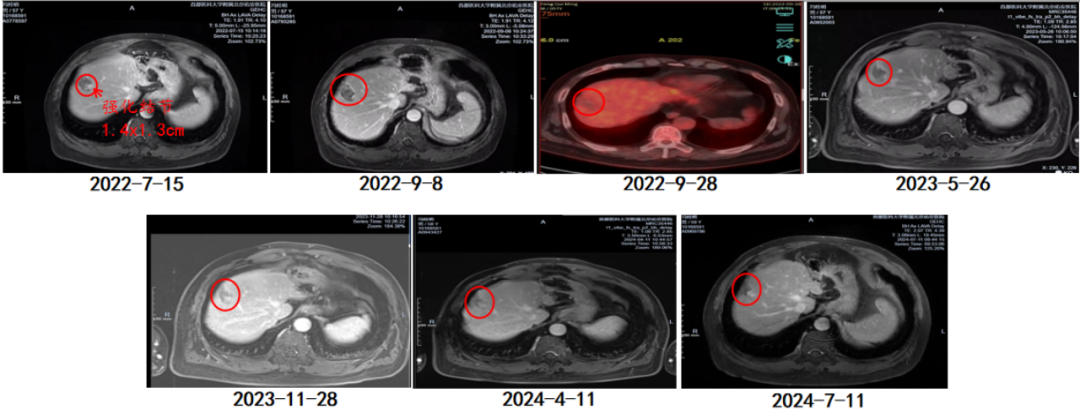
Imaging changes
Conclusion and Commentary
Postoperative recurrence is the most concerning issue for all patients with malignant tumors who have undergone surgical treatment, and it is also the greatest obstacle to achieving tumor cure. All patients with tumors have varying degrees of recurrence risk after surgical treatment. According to current standard treatment methods, for postoperative recurrence, reoperation or local minimally invasive treatment is usually employed, combined with systemic pharmacotherapy such as chemotherapy, targeted therapy, and immunotherapy. These treatment methods can effectively kill and inhibit tumor cells in the short term, but drug resistance cannot be avoided, and long-term efficacy cannot be achieved. Moreover, they have significant side effects, which can damage the immune system, hematopoietic system, and organ function. Therefore, none of these methods are ideal postoperative adjuvant treatments.



Scan QR code
Communicate with Professor Zhang Minghui's team

Click on the image to view past exciting content
