About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。

. The hardest part for cancer patients is the first 5 years. It's like a threshold; crossing it means a new beginning. But many people are not sure how to smoothly spend these 5 years. Is it all down to luck? Obviously not!
Today, let's take a look at the experience of a lung cancer patient who discovered metastasis just 9 months after surgery. It turns out that all of this is not random; many high-risk factors have been traceable early on, you just didn't see them!
2024 At the beginning of the year, Mr. Wang, who was 58 years old, found that he had persistent cough and expectoration, which lasted for more than a month. By 5 , he decided to go to the hospital to investigate what was wrong.

Upon further investigation, a mass lesion was found in the lower lobe of the left lung on CT scans, and it was quite large, measuring 6.1cmx4.8cm in its larger section. . Mr. Wang underwent a left lower lobectomy, lymph node dissection, and intercostal nerve block surgery that month.
○ Poorly differentiated adenocarcinoma is observed in the left lower lobe, with , and , with areas of showing neuroendocrine differentiation, .
○Lymph node metastasis was found. Metastatic lymph nodes were detected beside the left recurrent laryngeal nerve, with lymph nodes 2/3 showing cancer metastasis , with no metastasis in lymph nodes in other areas.
○No clear intravascular thrombus is observed, and the bronchial resection margin is negative. Staging considerations II B-III A stage .
○ Immunohistochemistry: Tumor cells : CK7( partial +), NapsinA(+), , TTF-1(+), , CK20(), , P40(-), , P63(-), , CK5/6(-), , Syna( A small number of (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+) (CD56(+).
After surgery, in 2024, , Mr. Wang underwent further treatment with pemetrexed + cisplatin chemotherapy to prevent metastasis and recurrence. However, the treatment was discontinued after only cycles due to , as his creatinine level had risen to 179 μ mol/L , making him unable to tolerate chemotherapy. Chemotherapy was no longer feasible, so Mr. Wang wanted to try targeted and immunotherapy drugs. However, genetic testing revealed no mutations, with a PD-L1test result of
At this point, Mr. Wang felt that he had already tried everything possible to treat his lung cancer, and considering that the disease was not too late in its stage, there should not be a big problem.
But unexpectedly, the disease progressed rapidly. In 2025, 2 months after Mr. Wang's surgery, a follow-up chest enhanced 9 month CT scan revealed lymph node enlargement in the
This issue has actually been studied by researchers, who have summarized the recurrence and metastasis patterns for patients with non-small cell lung cancer (NSCLC). A study focusing on patients with T1-T3aN0-N2M0 stage NSCLC after surgery revealed that the first peak of recurrence and metastasis risk, which is also the highest risk stage, occurs approximately months post-surgery. After this, the risk gradually decreases, reaching a second peak of recurrence and metastasis around months post-surgery. years post-surgery, with a third peak of recurrence and metastasis occurring thereafter. [1]
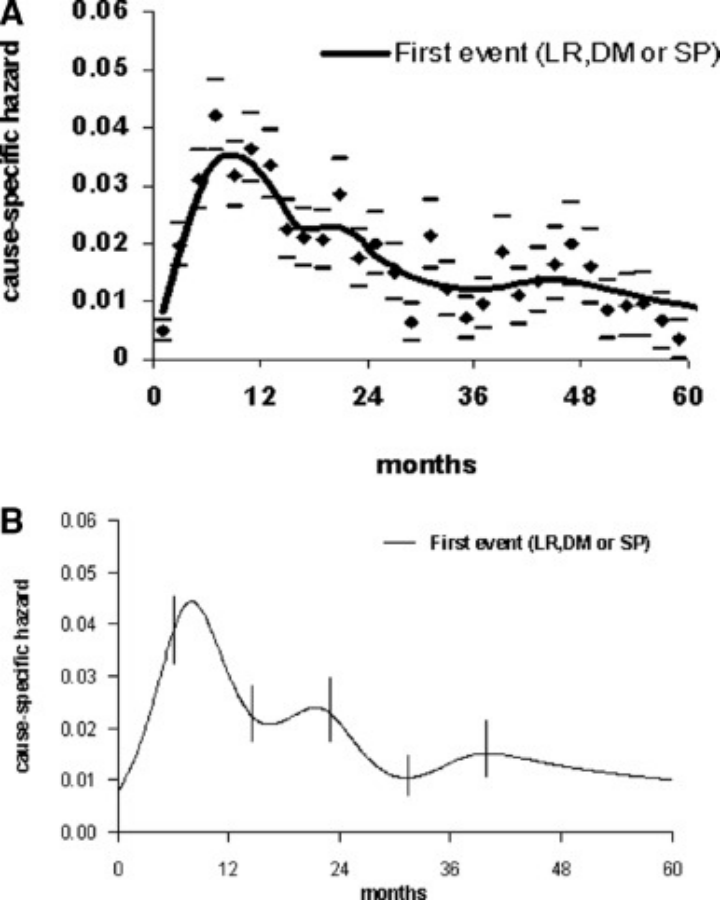
Mr. Wang's lung cancer recurred and metastasized 9 months after surgery, falling into the highest risk stage. This is not just bad luck; in fact, the risk has long been traceable. Here, I would like to remind everyone.
1、 Differentiation difference
TumorNotOnly viewVolume45/>Size, its differentiation degreeSimilarlyis important. Low differentiationCancer cells have stronger ability to divide, mutate, self repair, and resist chemotherapy and radiotherapy than highly differentiated cancer cells.
Neuroendocrine differentiation is also a tough player, growing fast, maturing early, and difficult to deal with.
Mr. Wang's Ki-67index is as high as 70%, indicating that approximately 70% of the cancer cells in the detected tumor tissue specimen are in an active division state, undergoing rapid replication. This rate is sometimes so high that even conventional chemotherapy cannot keep up.
2、 Lymph node metastasis< l-171/>/ Vascular cancer thrombus< l-185/>
Surgical removal of the primary lesion does not necessarily eliminate all hidden dangers. Lymph node metastasisand vascular cancer thrombusare important hidden dangers for cancer recurrence.
The lymphatic systemand the blood systemare important channels for cancer cells to spread throughout the body. When lymph node metastasisand vascular cancer thrombusoccursIndicates strong biological invasiveness of tumors, indicating that cancer cells have entered the stage of systemic dissemination,It is necessary to strengthen postoperative adjuvant therapy to encircle residual lesions.
3 , Limited treatment options
In clinical practice, it is often seen that patients like Mr. Wang terminate treatment due to excessive side effects of chemotherapy; they are unable to take targeted drugs due to mismatching mutant genes; and patients with PD-L1 expression negative are unable to benefit from immune checkpoint inhibitor therapy.
This means that patients will lose one or several highly effective anti-cancer weapons , and the clearance of residual cancer cells and the reduction of metastatic recurrence risk will also be greatly compromised, making the probability of cure uncertain.
After experiencing recurrence and metastasis, Mr. Wang once again embarked on the path of treatment. In 2025, , 3 , he switched to a new chemotherapy regimen consisting of albumin paclitaxel plus carboplatin plus bevacizumab. However, he still experienced bone marrow suppression, and even after reducing the dosage by half, he was only able to complete just two cycles of treatment before having to abandon it.
In 2025 , from 5 month to 6 month, he underwent carbon ion radiotherapy to address local metastatic lesions.
The lack of comprehensive treatment and the looming high-risk factors, made Mr. Wang and his family unable to sit still any longer. To address this gap in treatment, he reached out to Professor Zhang Minghui's team at Tsinghua University.
According to the analysis by Professor Zhang Minghui and the Lehexin Medical team:
① Mr. Wang's tumor exhibits low differentiation, neuroendocrine differentiation, Ki-67 (+ ), approximately 70%), , lymph node metastasis, and other indicators necessitate his classification as a high-risk group for recurrence and metastasis . Postoperative adjuvant therapy is not only necessary but also requires sufficient intensity.
② During the treatment process, Mr. Wang exhibited intolerance to chemotherapy, and no target was found for targeted therapy. The benefit possibility of PD-L1 is low. , conventional systemic treatment methods are ineffective, and there is an urgent need for new adjuvant treatment interventions. Sequential use of vNKT cell therapy has sufficient evidence of benefit. .
vNKTCell therapy, as an adoptive cellular immunotherapy, belongs to systemic therapy. It does not rely on PD-L1expression, nor does it require target matching
Experimental conditions: In the presence of vNKT cells, nearly all B16 tumor cells were killed after 16 hours!
vNKT cells are a special subset of T cells that possess both non-specific and specific recognition abilities for tumor cells. They can rapidly kill tumor cells. It also regulates the immune microenvironment within tumor tissues, killing inhibitory immune cellsMDSCs, and disrupts tumor immune evasion. It also has unique advantages inrebuilding a normal immune system, clearing residual cancer cells, and further preventing recurrence and metastasis.
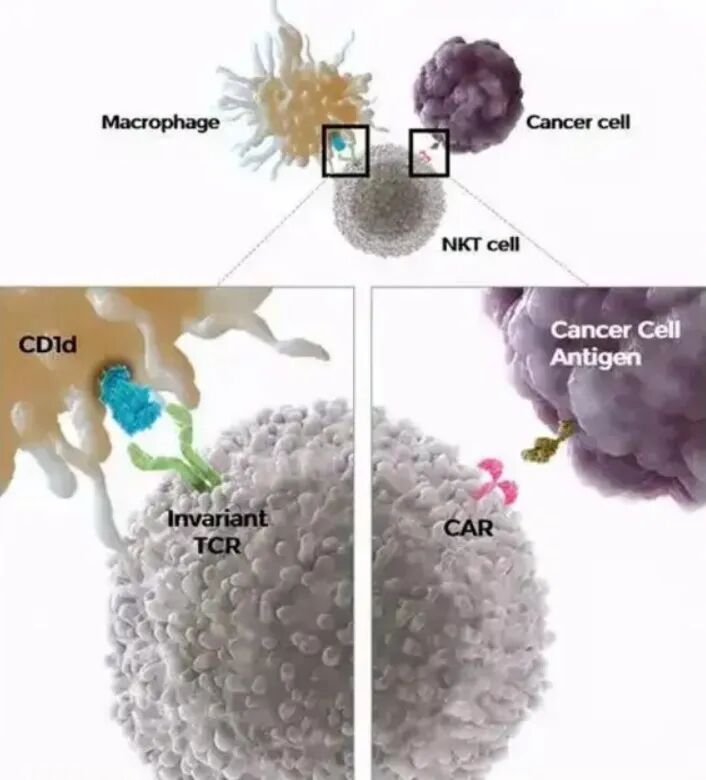
③ Mr. Wang has a high degree of intolerance to chemotherapy, making safety a crucial factor in his choice of alternative treatment methods. Compared to traditional chemotherapy and radiotherapy, vNKTcell therapy has minimal side effects, making it easier for patients to tolerate.
④ Currently, Mr. Wang has undergone resection of the primary lesion, and carbon ion radiotherapy after metastasis has addressed the local lesion. After reducing the tumor burden, it is a good opportunity for interventional vNKTcell therapy .
After listening to the analysis by Professor Zhang's team, Mr. Wang was full of expectations for vNKT cells. Therefore, he entered treatment in 2025, 6 month. After
Mr. Wang's experience once again confirms that "recurrence and metastasis are not dependent on luck. The hints of recurrence and metastasis have already been given, and those 'invisible' residual enemies have never truly left."
The surgical scalpel can remove visible tumors, but there are always a very small number of cunning cancer cells that can evade the pursuit of conventional treatment. They hide, disguise, and wait for the opportunity to make a comeback.
After surgery, a calm period of 9 months is not proof of cure, but rather the calm before the storm.
Fighting cancer is never a game of luck, but a protracted war that relies on scientific insight to gain the upper hand. Those who truly emerge victorious are those who dare to face "high-risk" and take the initiative. Precise monitoring and cutting-edge treatment are the strongest backing to help patients overcome the 5-year threshold.


Reference:
[1] Romano Demicheli, Marco Fornili, Federico Ambrogi, Kristin Higgins, Jessamy A. Boyd, Elia Biganzoli, Chris R. Kelsey, Recurrence Dynamics for Non – Small-Cell Lung Cancer: Effect of Surgery on the Development of Metastases, Journal of Thoracic Oncology, 2012 , 7(4) : 723-730. DOI : 10.1097/JTO.0b013e31824a9022.
Click to view past cases

