About Lehe
乐于心,和与众,与己乐,与人和; 心宽念纯,百病无生。


Esophageal cancer is one of the most common malignant tumors globally. According to the 2020 global cancer statistics, there were 604,000 new cases of esophageal cancer and 544,000 deaths. China is a high-incidence area for esophageal cancer. With the development of early diagnosis and treatment technologies, the mortality rate of esophageal cancer in China has shown a downward trend. The 5-year survival rate for early-stage esophageal cancer can reach over 90%. However, due to the fact that most patients are diagnosed at an advanced stage, the treatment outcome remains poor. The overall 5-year survival rate is only around 20%, making it a major malignant tumor that continues to threaten the health of Chinese residents.
Excessive drinking, smoking, nitrite intake, esophageal reflux, consuming hot foods, and drinking hot water are all associated with esophageal cancer. Genetic factors are also significant. If there is a history of esophageal cancer in immediate family members or multiple relatives, regular physical examinations should be conducted and exposure to high-risk factors should be avoided. Of course, even for the general population, it is important to try to eliminate the aforementioned habits and seek symptomatic treatment when necessary.

Overview of the illness
1. Mr. Zhao's pathological stage is ⅡB, with lymph node metastasis already present. In this case, the recurrence probability of simple surgical resection is extremely high. Therefore, adjuvant therapy should be actively pursued after surgery to further eliminate residual tumor cells and achieve the goal of controlling tumor recurrence.
2. Multiple studies suggest that postoperative adjuvant radiotherapy can improve the prognosis of patients with positive lymph nodes after undergoing simple surgery, and the efficacy of radiotherapy combined with chemotherapy is superior to that of radiotherapy alone. Currently, adjuvant therapy for esophageal cancer surgery mainly employs chemotherapy. However, for patients with esophageal cancer, chemotherapy has a low response rate and poor therapeutic effect, with an objective response rate of only 6%-8%. It can only exert a killing and inhibitory effect on tumor cells in the short term and is associated with drug resistance. Additionally, chemotherapy has significant side effects, causing severe damage to the immune system and hematopoietic system, and cannot achieve long-term efficacy. Therefore, it is not an ideal adjuvant therapy for postoperative patients.
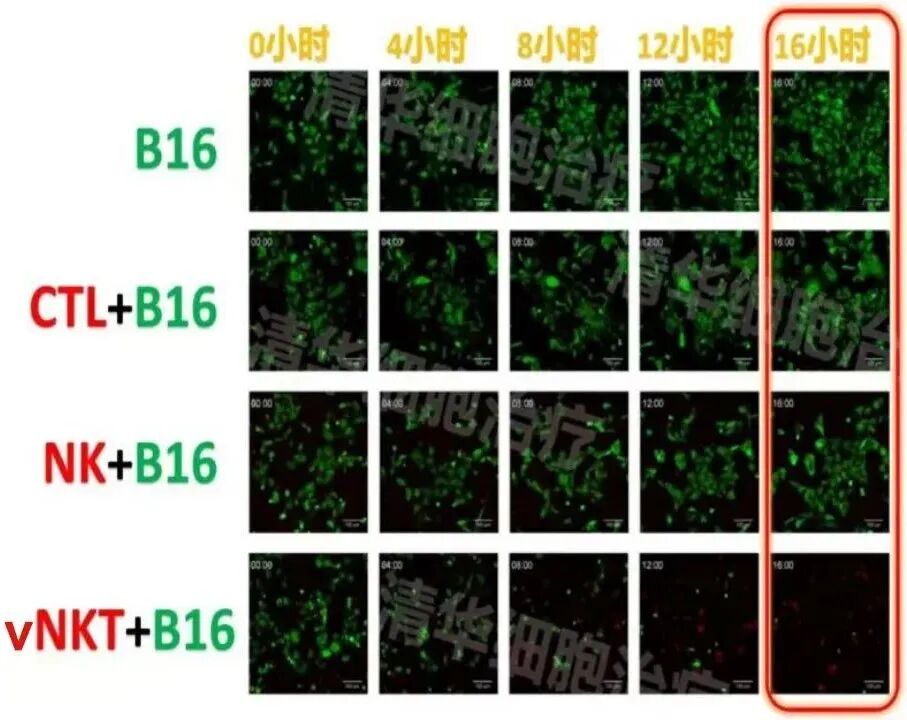
Experimental conditions: In the presence of vNKT cells, after 16 hours, nearly all B16 tumor cells were killed!
Professor Zhang provided Mr. Zhao and his family with a detailed introduction to the vNKT treatment technology and the treatment outcomes of previous cases, and answered Mr. Zhao's questions in detail. After thorough communication, Mr. Zhao and his family unanimously recognized the "strategic" thinking and "tactical" planning of Lehe team regarding tumor treatment, and began vNKT cell therapy on March 7, 2022. The first-stage treatment plan: 1 course/month, adjusted to 1 course/2 months in July 2023, and currently 16 courses have been completed (as of October 2024). Currently, the patient's condition is stable with no signs of recurrence or metastasis, and the patient is in good spirits, with good appetite and sleep, and a good quality of life.
Imaging changes
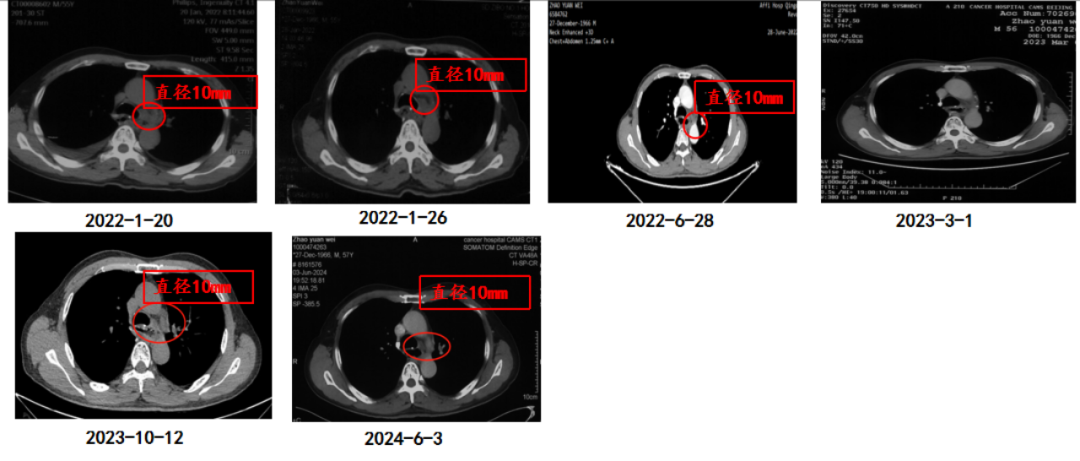
Conclusion and Commentary
Postoperative recurrence is the most concerning issue for all malignant tumor patients who have undergone surgical treatment, and it is also the greatest obstacle to achieving tumor cure. All tumor surgeries carry a certain degree of recurrence risk, especially for tumors that are discovered at a late stage, are large, or have a high degree of malignancy. Mr. Zhao's postoperative pathology indicated lymph node metastasis, which significantly increases the risk of postoperative recurrence. According to traditional treatment protocols, he should undergo chemotherapy and radiotherapy after surgery. However, after learning about the limitations and harmful effects of chemotherapy and radiotherapy on the body, Mr. Zhao rejected this treatment approach.
After scientific analysis and comparison, he ultimately chose vNKT cell therapy. He has been in stable condition for 3 years since the treatment, achieving ideal therapeutic effects. In this process, vNKT cell immunotherapy played an indispensable role in reducing the risk of recurrence and metastasis, providing patients with the possibility of achieving long-term tumor stability or even cure.



Scan QR code
Communicate with Professor Zhang Minghui's team

Click on the image to view the exciting content from previous issues
